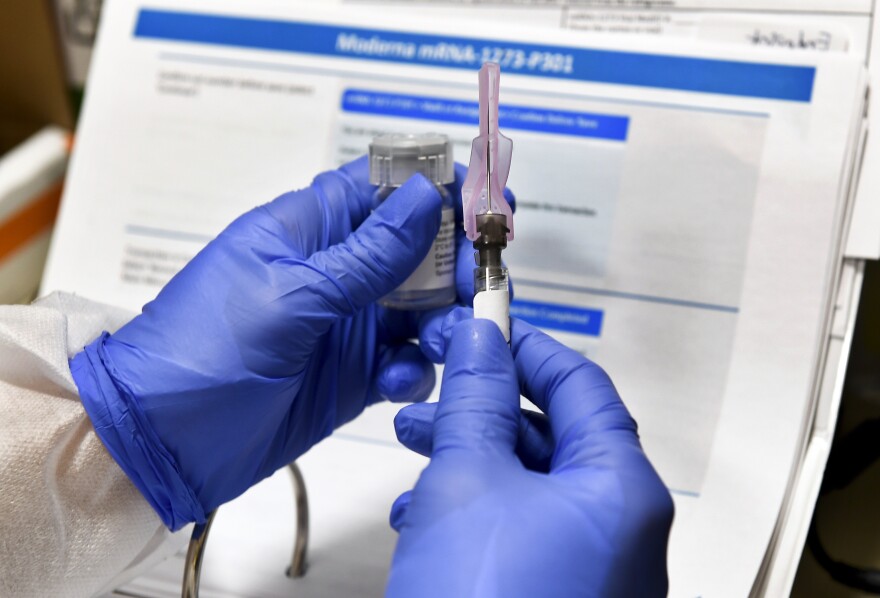
When a vaccine becomes available for COVID-19, who gets it first?
That’s the latest question VPR’s people-powered journalism project, Brave Little State, has set out to answer. It was asked by a Vermonter named Roger Stone. And no, he’s not that Roger Stone. Although this Roger Stone says he did used to get phone calls for the other guy, when they both lived in Manhattan.

Anyway, this Roger Stone is retired from the advertising industry.
“Oh, quite retired,” he tells me. “I'm 79 years old, and right there in the prime age group for having some bad things happen to you if you happen to contract COVID.”
Stone lives in in Bondville, a tiny village in the small town of Winhall. And he says there’s no Instacart where he lives. No for-profit delivery services. Not for food, not for meds. And, he says, policymakers haven’t done much to help older folks like him stay safe at home.
So when he heard the feds were starting to discuss how a vaccine should be distributed? Stone tuned in.
“And realized that it's really a question,” he says. “It's just like, not a slam dunk that the old people would get a high priority right behind health care workers and essential workers.”
That had him worried. Worried enough to write in to Brave Little State:
“What's on my mind is how the state is going to set priorities for the vaccines when they become available," Stone says. “How is this going to be settled out? Is there a committee? Is there a governor? How does that work?”
Subscribe to Brave Little State for free, so you never miss an episode:
Where vaccines are at
Alrighty. Let’s get up to speed on the global effort to get a vaccine for COVID-19 to folks like you and me.
According to a handy guide published by the New York Times, a number of teams began work on vaccines about eight months ago, in January. After testing on mice and monkeys, the first safety trials began in a small group of humans in March.
As of mid-August, there are more than 165 vaccines in various stages of development. About 30 are in human trials. Eight are in Phase 3 trials, being tested on tens of thousands of people for safety and effectiveness. Two have already been approved for limited use.
More from VPR: Confused About Antibodies? Let Our Comic (Featuring Many Llamas) Explain
And the federal government has been funding mass production of a number of vaccines. Optimists say one or more vaccines could be available to the public by the end of the year.
Others say sometime next year is more realistic. That’s really TBD. But whenever it is available, there probably won’t be enough for everyone, not right away. As for who will get access first? Roger Stone, and other older Vermonters ? They aren’t the only ones who wanna know.
Who gets priority?
Heidi Hopper, who works as a paraeducator in South Burlington’s elementary schools, hopes to get vaccinated sooner rather than later.
“I last year was diagnosed with non-Hodgkins Lymphoma,” she says. “I’m hoping that I would be on that list… coming from cancer, and working in schools.”

And although her treatment went well, and she is now one year cancer free, chemotherapy damages the immune system. This semester, while Hopper’s colleagues plan to be back in schools teaching in person, she’ll work from home.
“I would love to be back in school with people,” Hopper says. “You know, I'm a people-person, so it will be very hard for me if I don't get the vaccine and I'm home.”
Neither Hopper nor Stone think they should be first in line. In fact, almost everyone I talked to agreed those vaccines should be reserved for frontline health care workers.
But after that – if there really is a shortage –who is next? Other essential workers? Vermont’s elders? People with suppressed immune systems? What about people of color? In Vermont, Black people have gotten COVID-19 at 11 times the rate of white people.
Giving priority to high-risk populations in this case would involve looking at racially diverse communities, based on the very worrying racial disparity that we have.
More from VPR: Race, COVID-19 And Health Disparities In Vermont
Maria Mercedes Avila is an associate professor of pediatrics and the health equity liaison at the Larner College of Medicine at UVM. She joins a chorus of medical professionals who say some racial minorities should also get priority access.
“Children under nine who tested positive for COVID-19, of those children, 68% are children who are racially diverse,” Avila says. “That's a very alarming statistic for the second whitest state in the country.”
Indeed. So many groups have valid reasons to want to be near the front of the COVID-vaccine line.
How to decide?
Christine Finley, the immunization program manager at Vermont’s Health Department, is pretty familiar with the vaccine distribution process. She’s one of 31 liaisons to the Centers for Disease Control’s standing Committee on Immunization Practices -- or ACIP. It’s the group that writes federal guidelines for vaccines.
Finley represents immunization managers across the country, alongside the American Academy of Pediatrics, Academy of Family Physicians, the Association of State and Territorial Health Officers, U.S. Department of Veteran Affairs, Indian Health Service and more.
Those liaisons and 15 voting members -- almost all are doctors -- break out into more than dozen work groups to look at all aspects of vaccines: their safety, their efficacy, who should get it, when. The committee then writes and votes on vaccine guidance, which it sends to the CDC.
“And that's the guidance that is expected to be followed by all health care providers,” Finley says.
So is any of this process different for COVID-19? Short answer: Yes.
“Everything's different for COVID,” Finley says with a laugh.
Loading...
For one, Finley’s group has been meeting monthly, online, rather than the usual three times a year in Atlanta. And, she says, the information is coming from vaccine researchers with a speed that’s all together new.
But most different is that this time, there’s a second group doing similar work at the National Academies of Science, Engineering and Medicine. They are focusing especially on issues of equity.
And somehow, by October, Finley says, these two groups hope to issue federal guidance.
After that, whenever the vaccine is available, the federal government will pay for and distribute it to each jurisdiction based on population size and other factors. That’s according to the CDC.
Once that happens, it’ll be up to people like Christine Finley to figure out how to get the right number of doses to the people at the top of the list.
The ethics
Whoever those people are, many will likely be getting vaccine doses from UVM Medical Center, Vermont’s largest medical provider and the largest employer in the state.
Among those employees is Tim Lahey, a vaccine researcher and the medical center’s director of ethics. He says hospital leadership has asked the state to convene stakeholders to discuss vaccine access.
“I know that conversations about the fair distribution of the vaccine are already starting,” he says.
I wondered about the motivation – whether UVM Medical Center was being very attentive to health care workers’ safety, or if it was more about them having to deal with the public, and therefore wanting some guidance?
Lahey’s answer: Yes.
He says hospitals don’t have to deal with scarcity that often. And there will a lot of scrutiny around vaccine distribution. Hospital officials don’t want to be the only ones involved.
Loading...
Lahey, of course, is trained in medical ethics -- he understands as well as anyone the challenges facing the committee members writing the vaccine guidance. And, in his mind, vaccines are different from organ transplants or ventilators. He says you can’t just think about who is most at risk of dying.
“Because if we found out that you can't contain the epidemic without vaccinating people in their 20s and 30s who are perfectly healthy, then we have to prioritize those people, because the point is to save lives,” he tells me.
And then Lahey brings up another complicating factor, which actually works against older people like Roger Stone and immunocompromised people like Heidi Hopper:
“Almost all vaccines have less effective responses from people who are immune compromised and elderly,” Lahey says. “So you get into this interesting conundrum where elderly people need protection from influenza the most. They need protection from COVID-19 the most. But they're also less likely to have a great response to the vaccine. And so the ideal population-level response probably is a combination of giving it to people who are most at high risk and giving it to people who are most likely to respond.”
This was news to me. And this concept of prioritizing at the population level, rather than the individual? Lahey says it’s one reason certain racial minorities should get prioritized for vaccine.
He says that’s different, however, when you’re talking about ventilators. At 2 a.m. when two people are vying for one ventilator, you really can’t know which of those people has suffered more injustice.
“Vaccination is different. We know that race is a marker of risk of severe COVID-19,” Lahey says. “And we want to distribute the vaccine preferentially to people who are most at risk so that we can save the most lives possible. And vaccination is a population-level intervention.”
Ideally, he says, there will be enough vaccine for everyone to access ASAP. That is still a possibility. But if there isn’t, it’s not really up to UVM Medical Center to decide who gets priority. It’s up to the CDC – and the National Academies of Science, and their committees— who are in the midst of eternal video conferences, hashing all this out.
Loading...
Not everybody wants to go first
But wait. All of this concern about who gets the vaccine first? Its premise is an assumption. One I didn’t think much about until I talked to Linda Goodman.
“I have a rare blood cancer called Waldenstrom's, it's a non-Hodgkin's lymphoma,” she tells me.
Goodman is in the same support group as Heidi Hopper, the cancer survivor who works in elementary schools. Only Goodman is not gunning to be first in line for a COVID-19 vaccine.
“It’s an interesting question that you ask,” Goodman says. “The question is, who is it safe for, more than who should have priority? And when the vaccine came out, I would not get it initially until it'd been out for X period of time, so I knew what the side effects would be.”

Goodman was open to the vaccine until she heard a segment on a SiriusXM radio station called Doctor Radio. That’s where she learned that even though the vaccines are going through the traditional Phase 3 30,000 person clinical trials, very rare side effects, or those affecting very small segments of the population, may not be understood until hundreds of thousands of people have received the vaccine.
And because of her cancer, Goodman says -- she doesn’t want to go first. Plus, she says, she’s lucky.
“I have this amazing home that looks out into many, many acres, including water,” she said.
And Goodman has a husband who does the shopping, and keeps her company. She’s willing to be cloistered away.
But what she brought up — this fear that the vaccine won’t be safe? It’s more prevalent than I had understood. And it’s more prevalent than doctors and public health officials like Christine Finley would like.
“They named the whole piece about the vaccine on the federal level, ‘Operation Warp Speed,’” Finley says. “I don't think there could be a worse name that you could name something.”
She adds: “Because I think that it just says, ‘Oh, gosh, they're really rushing it.’ And it misses what's going on. In the trials that they're doing, the standard is that you want 30,000 people in those trials. They are going to have 30,000 people. They are not cutting the size of the population that is going to be in the trials.”
Finlay also notes that in a poll done by the Associated Press and University of Chicago, only half of American adults said they would definitely get a COVID-19 vaccine when it comes out.
“We need to do better than that if we want to achieve herd immunity,” Finley says.
As a liaison to the CDC working group, Finley is watching the sausage get made. And, she says, it’s made her confident the vaccine will be safe.
In the meantime, she and the committees figuring all this out are left with two contradictory but equally important mandates: Figure out how to save the most lives with a small amount of vaccine, and then convince people to come and get it.
Subscribe to Brave Little State for free, so you never miss an episode:

Thanks to Roger Stone for the great question.
If you have a question about COVID in Vermont, or anything else, ask it at bravelittlestate.org. While you’re there you can sign up for our newsletter, and vote on the question you want us to tackle next. We’re on Instagram and Twitter @bravestatevt.
This episode was produced by Emily Corwin, with editing from Mark Davis.
Brave Little State is a production of Vermont Public Radio. Our digital producer is Elodie Reed, and we have engineering support from Chris Albertine. Ty Gibbons composed our theme music; other music by Blue Dot Sessions.